The Science Behind In Vitro Fertilization: How It Works
Introduction
In recent decades, In Vitro Fertilization has transformed the landscape of reproductive medicine, offering hope to individuals and couples facing infertility. While IVF is often discussed in emotional or practical terms, the science behind it is equally fascinating. It combines biology, endocrinology, and advanced laboratory techniques to assist conception outside the human body.
Understanding how IVF works can make the process feel less overwhelming and more approachable. This guide breaks down the science step by step, explaining what happens at each stage and why it matters.
What Is In Vitro Fertilization?
IVF is a medical procedure in which fertilization occurs outside the body, typically in a specialized laboratory. The term “in vitro” means “in glass,” referring to the controlled environment in which the egg and sperm are combined.
In a natural pregnancy, fertilization occurs in the fallopian tubes. In IVF, this step is bypassed, allowing doctors to directly facilitate fertilization and monitor early embryo development before transferring it into the uterus.
The Role of the Reproductive System
To understand IVF, it helps to know how natural conception works. Each month, a woman’s ovaries release an egg during ovulation. If sperm is present, fertilization may occur, forming an embryo that travels to the uterus and implants in the uterine lining.
IVF replicates and enhances this process using scientific intervention. It focuses on four key elements:
- Egg production
- Sperm collection
- Fertilization
- Embryo implantation
Each of these steps is carefully controlled to increase the chances of a successful pregnancy.
Step 1: Ovarian Stimulation
The first stage of IVF involves stimulating the ovaries to produce multiple eggs instead of just one. This is done using fertility medications that mimic natural hormones such as Follicle-Stimulating Hormone and Luteinizing Hormone.
These hormones encourage the development of several follicles, each containing a potential egg. Producing multiple eggs increases the likelihood of successful fertilization and viable embryos.
Doctors monitor this phase using blood tests and ultrasounds to track hormone levels and follicle growth.
Step 2: Egg Retrieval
Once the eggs have matured, they are collected through a minor surgical procedure known as egg retrieval. This process is typically guided by ultrasound and performed under sedation.
A thin needle is used to retrieve eggs from the follicles in the ovaries. The collected eggs are then immediately transferred to a laboratory, where they are evaluated for quality and readiness for fertilization.
Step 3: Sperm Collection and Preparation
At the same time, a sperm sample is collected from the male partner or a donor. The sample undergoes a process called sperm washing, which separates healthy, motile sperm from other components.
The goal is to select the most active and structurally normal sperm to improve the chances of fertilization.
Step 4: Fertilization in the Lab
Fertilization can occur in two primary ways:
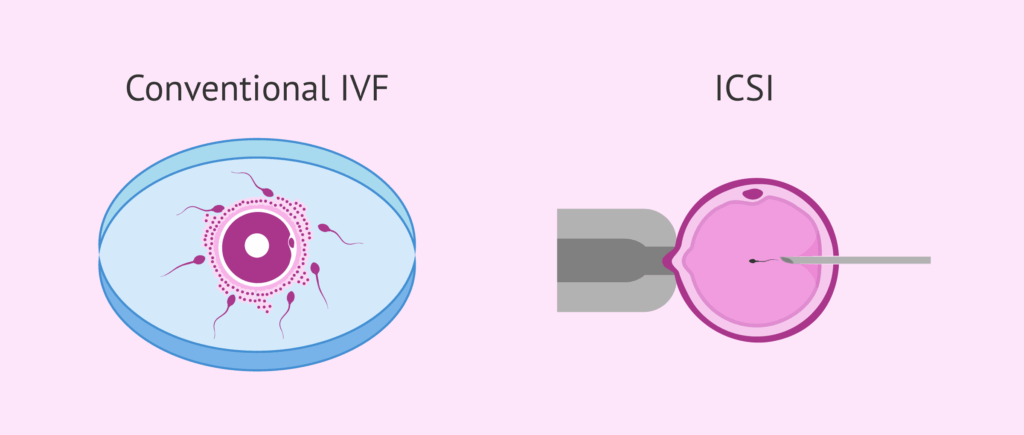
Conventional IVF
In this method, eggs and sperm are placed together in a laboratory dish, allowing fertilization to happen naturally.
Intracytoplasmic Sperm Injection
Here, a single sperm is directly injected into an egg using a fine needle. This technique is often used in cases of male infertility or previous fertilization failure.
After fertilization, the resulting cells begin dividing and developing into embryos.
Step 5: Embryo Development
Fertilized eggs are monitored over several days as they develop into embryos. During this time, embryologists assess their growth, structure, and quality.
By day five or six, some embryos reach the blastocyst stage. At this point, the embryo has differentiated into distinct cell types and is more likely to implant successfully in the uterus.
Step 6: Embryo Transfer
In the next stage, one or more healthy embryos are selected and transferred into the uterus. This procedure is relatively simple and does not require anesthesia.
The goal is for the embryo to implant into the uterine lining, leading to pregnancy. This step mimics the natural process that occurs after fertilization in the body.
Step 7: Implantation and Pregnancy
If the embryo successfully implants, it begins producing the hormone Human Chorionic Gonadotropin. This hormone supports the early stages of pregnancy and is what pregnancy tests detect.
About two weeks after the embryo transfer, a blood test is conducted to confirm whether implantation has occurred.
The Role of Technology in IVF
Modern IVF relies heavily on advanced technology to improve outcomes. High-resolution imaging, controlled incubators, and precise laboratory conditions all play a role in supporting embryo development.
In some cases, additional techniques may be used, such as genetic testing of embryos to identify chromosomal abnormalities. This can help select embryos with a higher chance of successful implantation and healthy development.
Factors That Influence IVF Success
IVF success is influenced by several scientific and biological factors, including:
- Age and egg quality
- Sperm health
- Uterine environment
- Hormonal balance
- Lifestyle factors
Younger individuals generally have higher success rates due to better egg quality, while underlying medical conditions can also affect outcomes.
Risks and Considerations
While IVF is generally safe, it is not without risks. Potential complications include ovarian hyperstimulation, multiple pregnancies, and emotional stress.
For younger individuals, it’s important to understand that IVF is a complex medical procedure that should only be pursued under professional guidance. It is not a quick or guaranteed solution but rather a carefully managed scientific process.
The Future of IVF
Research in reproductive medicine continues to evolve. Scientists are exploring new ways to improve embryo selection, enhance implantation rates, and reduce risks.
Emerging technologies, such as artificial intelligence in embryo assessment and improved genetic screening, may further refine IVF outcomes in the coming years.
Also Read: IVF and Age: How Fertility Changes Over Time
Final Thoughts
The science behind IVF is a powerful example of how medicine and technology can work together to overcome biological challenges. By replicating and enhancing natural reproductive processes, IVF offers a pathway to parenthood for many who might not otherwise have that opportunity.
Understanding how IVF works not only demystifies the process but also highlights the incredible precision and care involved at every step. As research advances, the future of IVF looks increasingly promising, with the potential to make fertility treatments more effective, accessible, and personalized.
